Related links: The Endocrine Disrupter Scare | ATSDR Atrazine Profile
2-Minute Junking: Atrazine lowers testosterone?
Related links: The Endocrine Disrupter Scare | ATSDR Atrazine Profile
Related links: The Endocrine Disrupter Scare | ATSDR Atrazine Profile
Related links: AP article | Louisiana Tumor Registry report | 2003 Industrial Corridor study
Related links: WaPo article | EPA on PFAS | New York Times exposure | WaPo 3M lawsuit
This morning I came across this story in The Guardian.
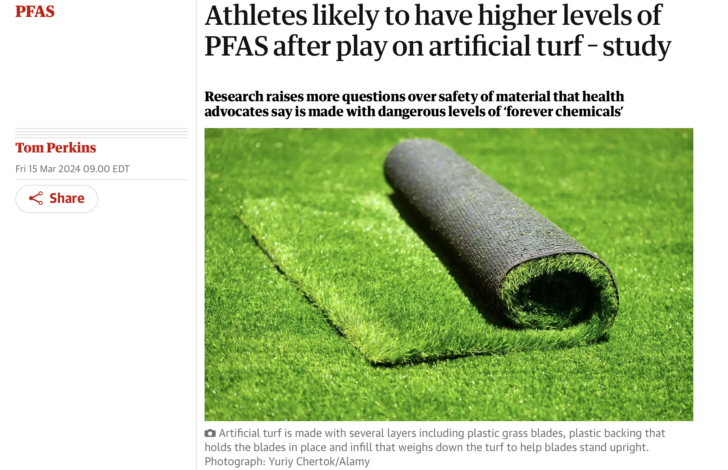
Continue reading Industry document says PFAS are ‘highly toxic’?
One of the of the first regulatory controversies I was involved in when I started working on environmental issues in 1990 was the formaldehyde risk assessment. The controversy continues to this day with an impatient EPA trying to ram through a rigged risk assessment. That alone should tell what you need to know about any junk science-fueled alarm over formaldehyde — a much-studied and well-understood chemical. Here is a fact sheet on the EPA formaldehyde railroad prepared by the American Chemistry Council. Also check out the related letter from ACC, and this letter from Ohio Congressman Mike Carey to the rogue EPA.
A new study claims that women with high PFAS levels in their blood samples reached menopause two years earlier than those with lower levels. Credible?

JunkScience has been on top of the always-bogus endocrine disrupter scare since its beginning in March 1996.
Now, JunkScience.com has compiled “The Endocrine Disrupter Scare,” a history of the scare.

JunkScience.com friend, the great Stan Young scores a letter in the Wall Street Journal in support go Steve Milloy’s op-ed from earlier this week.

Continue reading Stan Young backs Milloy Wall Street Journal op-ed on endocrine disruptors
My op-ed in today’s Wall Street Journal about the debunking of the BPA scare.

Let’s review the nonsense in today’s New York Times op-ed by notorious junk scientist goofballs Phil Landrigan (Mt. Sinai) and Lynn Goldman (George Washington University).


Continue reading Children are NOT more sensitive /vulnerable to chemicals in the environment