This meta-analysis does NOT show that hydroxychloroquine + azithromycin (HCQ-AZI) increases mortality.

The reported associations for HCQ-AZI are all noise level, zero correlations.
The meta-analysis has significant limitations:

No doubt this study will be used for political reasons to attack President Trump. There is no scientific basis for this.
The media release is below. The study is here.
###
New analysis shows hydroxychloroquine does not lower mortality in COVID-19 patients, and is associated with increased mortality when combined with the antibiotic azithromycin
EUROPEAN SOCIETY OF CLINICAL MICROBIOLOGY AND INFECTIOUS DISEASES
A new meta-analysis of published studies into the drug hydroxychloroquine shows that it does not lower mortality in COVID-19 patients, and using it combined with the antibiotic azithromycin is associated with a 27% increased mortality. The study is published in Clinical Microbiology and Infection, the official journal of the European Society of Clinical Microbiology and Infectious Diseases (ESCMID).
“This meta-analysis shows that hydroxychloroquine alone is not effective for the treatment of COVID-19 patients and that the combination of hydroxychloroquine and azithromycin increases the risk of mortality,” say the authors who include Thibault Fiolet, Center for Research in Epidemiology and Population Health, INSERM, Institut Gustave Roussy and Paris-Sud 11 University/Paris-Saclay University, Paris, France. “These data support current clinical recommendations such as those of the US National Institutes of Health (NIH) which do not recommend the use of hydroxychloroquine alone or in combination with azithromycin for COVID-19 patients.”
Chloroquine is used to prevent and treat malaria, while hydroxychloroquine is a less toxic metabolite of chloroquine and is used to treat rheumatic diseases such as systemic lupus erythematosus (SLE), rheumatoid arthritis (RA), juvenile idiopathic arthritis (JIA) and Sjogren’s syndrome. Hydroxychloroquine in particular has received extensive media coverage since the outbreak of the SARS-CoV-2 pandemic as a potential treatment for COVID-19. Azithromycin is used to treat a wide range of bacterial infections, but has also been promoted as a potential treatment for COVID-19 due to its alleged antiviral or anti-inflammatory properties.
In this new analysis, the authors searched for studies that assessed chloroquine or hydroxychloroquine with or without the antibiotic azithromycin. The authors found 29 articles that met their criteria, all except one of which were conducted on hospitalised patients and evaluated the effects of hydroxychloroquine with or without azithromycin.
Among the 29 articles, 3 were randomised controlled trials, one was a non-randomised trial and 25 were observational studies, including 11 with a ‘critical’ risk of bias and 14 with a ‘serious or moderate’ risk of bias*. After excluding studies with a critical risk of bias, the meta-analysis included 11,932 patients in the hydroxychloroquine group, 8,081 in the hydroxychloroquine with azithromycin group and 12,930 in the control group (who received neither drug).
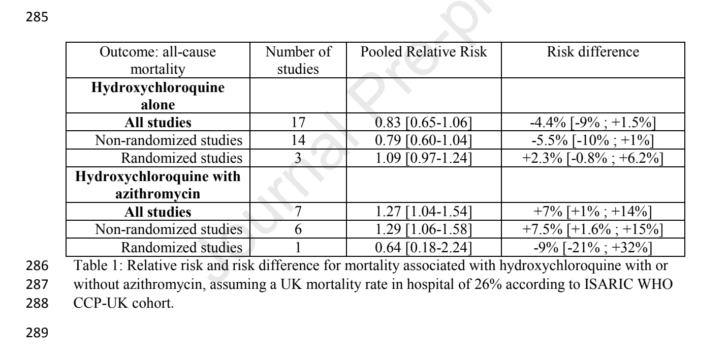
The results showed that hydroxychloroquine was not associated with mortality, either in all trials combined, or in separate analyses of randomised controlled trials or observational studies. The relative risk of death for use of hydroxychloroquine was 17% lower than controls for all studies combined, but 9% higher in randomised controlled trials. In both cases, these results were not statistically significant.
However, the combination of hydroxychloroquine and azithromycin in patients with COVID-19 was associated with a statistically significant 27% increase in mortality compared with controls. The authors say: “These results confirm the preliminary findings of several observational studies which have shown that the combination of hydroxychloroquine and azithromycin might increase the risk of acute, life-threatening cardiovascular events.”
The authors discuss limitations of their work which include the differing levels of COVID-19 disease severity across patients and also the actual definition of severity. Furthermore, most of the studies included were observational studies (not designed to find a causal relationship). Finally, this meta-analysis did not include results from the European DisCoVeRy trial and the WHO Solidarity trial that are not yet published or communicated (but both have already discontinued their hydroxychloroquine arms).
The authors conclude: “There is already a great number of studies that have evaluated hydroxychloroquine alone or in combination and it seems unlikely at this stage that any efficacy will ever emerge. Our results suggest that there is no need for further studies evaluating these molecules, and the European DisCoveRy and WHO international Solidarity clinical trials have already discontinued treatment arms using hydroxychloroquine.”
###